Beta Cell Preservation
YOUR GUIDE TO
Beta Cell Preservation
in Type 1 Diabetes
A simple guide for patients, families, and caregivers
What you will learn in this guide
- Section 1: Why Preserving Your Beta Cells Matters
- Section 2: Why Beta Cell Function Is So Important in Type 1 Diabetes (T1D)
- Section 3: Myths vs Facts—What Can YOU Do?
- Section 4: Questions to Ask Your Healthcare Team
- Section 5: Treatments That May Help Protect Beta Cells
This guide uses simple words. You do not need a medical background to understand it. If you see a word you don’t know, look for the explanation in the same paragraph.
SECTION 1: Why Preserving Your Beta Cells Matters
First, what is a beta cell?1
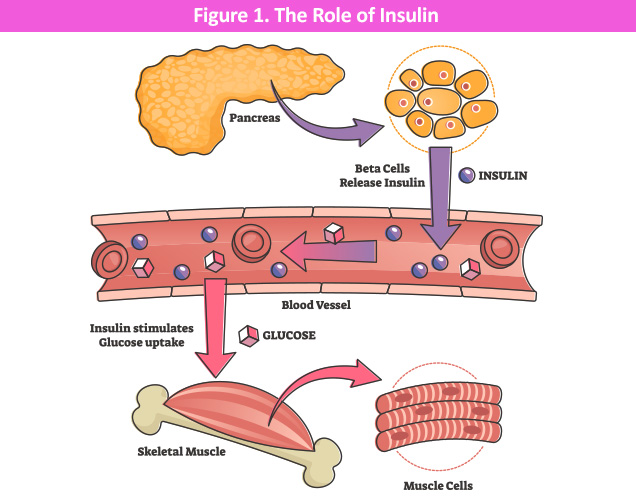
Your pancreas is an organ in your abdomen. Inside it are tiny groups of cells called islets. Inside those islets are special cells called beta cells.
Beta cells have 1 very important job: They make insulin.
Insulin is like a key. It opens the doors to your body’s cells so that sugar (glucose) from the food you eat can get inside and give you energy. Without insulin, sugar stays stuck in your blood and your cells don’t get the fuel they need.
The simple version
Beta cells = the factory that makes insulin.
In type 1 diabetes (T1D), the body’s own immune system attacks and destroys these beta cells.
This is like the factory being slowly shut down.
Once most beta cells are gone, your body cannot make its own insulin anymore.
So why does saving beta cells matter so much?1,2
When you—or your child—is first told they have T1D, some beta cells are still alive. They are still working, even if just a little. This is called the “honeymoon period” or residual (leftover) beta cell function.
Medical research shows that keeping even a small number of working beta cells can make a BIG difference in daily life with T1D. Here is why:
Did you know?
Studies show that people with T1D who keep even a tiny bit of beta cell function have up to 65% fewer dangerous low blood sugar events.
That’s like going from getting a scary low blood sugar 10 times a year down to just 3 or 4 times.3
SECTION 2: Why Beta Cell Function Is So Important in T1D
The difference between a little insulin and none2,4
Think of it this way: Imagine you are rowing a boat across a lake. You need to get to the other side (good blood sugar control). If you have NO oars at all, it is very hard—you are pushed around by wind and waves (big blood sugar swings).
Now imagine you have just 1 oar—not perfect but so much better! You have some control. You can steer. You can adjust. That is what a small amount of remaining beta cell function does. It acts like that 1 oar.
How your body uses leftover insulin2,4
Even when beta cells are mostly destroyed in T1D, many people—especially soon after diagnosis—still have some working beta cells left. These cells release tiny amounts of insulin in response to food. This is called “residual” (leftover) beta cell function.
Here is what that small amount of insulin can do:
- Help smooth out blood sugar spikes after meals
- Protect against dangerous lows, especially overnight
- Reduce the amount of injected insulin needed
- Help the body’s blood sugar-lowering response work better overall
- Reduce the chance of a serious condition called diabetic ketoacidosis (DKA)
A real-world example from research
Scientists followed people with T1D for over 30 years in a large study (called the Diabetes Control and Complications Trial/Epidemiology of Diabetes Interventions and Complications [DCCT/EDIC] study).
People who kept some beta cell function had:
- 50% lower risk of eye problems (retinopathy)
- 39% lower risk of kidney problems (nephropathy)
- 65% fewer dangerous low blood sugar events (severe hypoglycemia)
- Better blood sugar control overall (lower A1C levels)
Even very small amounts of leftover beta cell function helped—there was no level too small to make a difference!3,5
What happens to beta cells over time in T1D?2,4
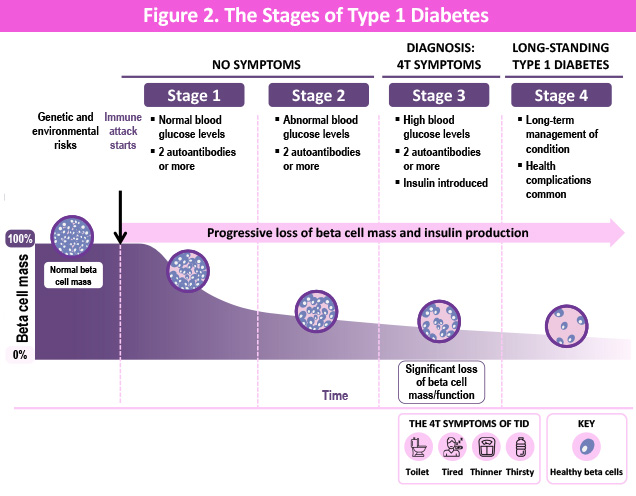
0In T1D, the immune system mistakes beta cells for enemies. It sends white blood cells to attack them. The rate of this attack is different for everyone, typically occurring faster in children and adolescents versus adults. For most people, this can happen quietly, often for years before the first symptoms show up.
By the time T1D is diagnosed, most beta cells are already gone—but not all. Studies show that at the time of diagnosis, about 20 to 30 out of every 100 beta cells may still be alive and working.
After diagnosis, the immune system usually keeps attacking. Without treatment, these remaining beta cells die off over months to a few years. This is why that window of time right after diagnosis is so important—it may be the best chance to step in and protect what is left.
Adapted from Breakthrough T1D.
The window of opportunity2,4
Right after a T1D diagnosis (and even before symptoms start) is the BEST time to protect beta cells.
The earlier we act, the more cells we can save.
This is why researchers are working hard to find treatments that can be given early—even before symptoms appear.
SECTION 3: Myths and Facts—What Can YOU Do?
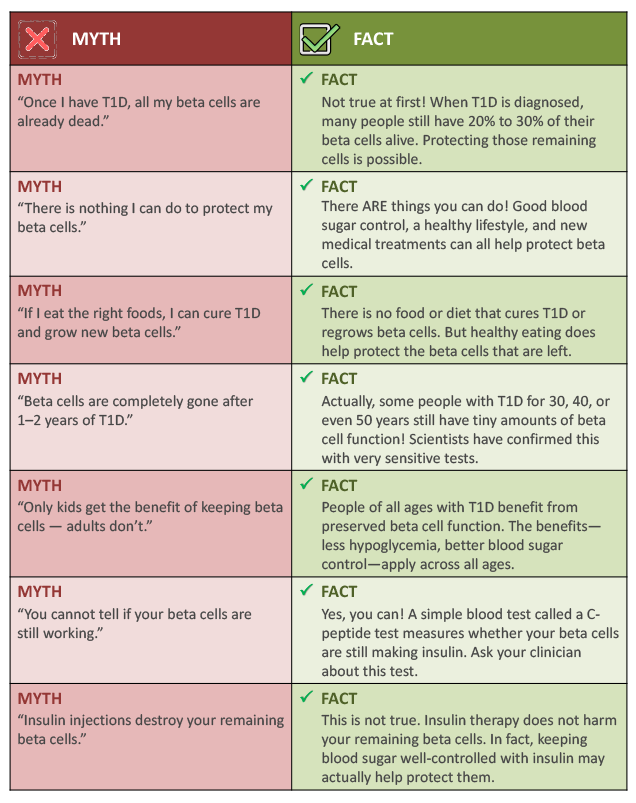
Common myths vs real facts about beta cell preservation6-9
There is a lot of confusing information out there about beta cells and T1D. Let’s clear some of it up.
What CAN you do right now to help your beta cells?6-9

1. Keep your blood sugar as steady as possible.
This is the #1 thing you can do.
When blood sugar swings wildly up and down, it creates extra stress on beta cells. This is sometimes called “glucotoxicity”—basically, too much sugar in the blood is toxic to beta cells.
Good control does NOT mean perfect control. It means working with your care team to reduce big highs and lows.
Tools such as continuous glucose monitors (CGMs) and insulin pumps can help a lot.
Research from the DCCT study showed that people who used intensive insulin therapy (keeping blood sugar closer to normal) preserved more beta cell function than those on standard therapy.

2. Get diagnosed early—and act quickly.
The sooner T1D is caught, the more beta cells may still be alive.
- Screening tests for T1D-related autoantibodies (the “warning signals” in the blood) can catch T1D before symptoms appear
- If you have a family member with T1D, ask about autoantibody screening programs such as ASK or TrialNet. These are often FREE
If a new diagnosis happens: Talk to your clinician right away about whether a disease-modifying treatment might be right for you.

3. Eat well and stay active.
No specific diet regrows beta cells—but overall healthy habits reduce inflammation in the body.
- A balanced diet with plenty of vegetables, whole grains, and lean protein helps keep blood sugar steadier
Regular physical activity helps insulin work better in the body (lowers “insulin resistance”).
- Aim for at least 30 minutes of movement most days—walking, swimming, biking, playing outside all count
Avoid long stretches of sitting—get up and move every hour or so

4. Avoid getting sick—protect your immune system.
Infections and illness can trigger more immune system activity, which can speed up beta cell loss.
- Stay up-to-date on vaccines (including flu shots and COVID vaccines)—infections can make T1D harder to control
- Wash hands often
- Avoid people who are sick when possible
- Manage stress—stress hormones can raise blood sugar AND ramp up immune system activity

5. Ask about clinical trials.
The MOST powerful way to help protect your beta cells right now may be to join a clinical trial.
Clinical trials test new medicines that could slow or stop the immune attack on beta cells.
Joining a trial helps YOU and helps future generations of people with T1D.
Ask your clinician or visit Breakthrough T1D (breakthrought1d.com), TrialNet (trialnet.org), or ClinicalTrials.gov to find trials near you.
Many trials are FREE to join, and some provide travel reimbursement.
IMPORTANT: None of the lifestyle steps above replace medical treatment. They work ALONGSIDE your insulin therapy and any disease-modifying treatment your clinician recommends. Always talk to your healthcare team before making big changes.
SECTION 4: Questions to Ask Your Healthcare Team

You—or your child—are the most important person in any conversation with your clinician or care team. Do not be afraid to ask questions. Good clinicians LOVE when patients ask questions—it means you are engaged and paying attention.
Here are some important questions about beta cell preservation to bring to your next appointment. Print this page and bring it with you!
Do I (or does my child) still have any working beta cells? How do you know?
Ask about a test called a C-peptide test. This simple blood test measures whether beta cells are still making insulin. Knowing this can help guide your treatment plan and whether new therapies might help.
Is a C-peptide test right for me right now? When should it be done?
C-peptide is most useful soon after diagnosis, or when your team is considering whether to add a new type of treatment. Ask when and how often you should be tested.
Am I (or is my child) a good candidate for a disease-modifying therapy such as teplizumab
There is now an US Food and Drug Administration (FDA)-approved medication that can slow T1D progression in people who have been recently diagnosed or are in the early stage before clinical diagnosis. Ask if this applies to your situation.
Are there any clinical trials we should know about?
Research on new beta cell–protecting treatments is happening right now. Your clinician may know of trials nearby. You can also ask about TrialNet—a free screening and research program for people with T1D and their relatives.
How can I tell if my beta cells are still working, and does it change my treatment plan?
Understanding your C-peptide level can change recommendations for insulin dosing, pump use, and adjunct therapies. Ask how this information will be used in YOUR specific care plan.
What blood sugar range should I aim for to best protect my remaining beta cells?
Understanding your C-peptide level can change recommendations for insulin dosing, pump use, and adjunct therapies. Ask how this information will be used in YOUR specific care plan.
Should my family members be screened for T1D-related autoantibodies?
First-degree relatives (parents, brothers, sisters, children) of someone with T1D have a higher risk of developing it too. Early detection can open the door to treatments BEFORE full T1D develops. Ask about options for screening, like the TrialNet or ASK programs.
What signs indicate the status of my beta cell function—whether they’re still working or have stopped?
Your clinician can explain what to watch for such as changes in how much insulin you need, blood sugar patterns, or C-peptide test results. Knowing the signs helps you stay informed.
Are there any foods, supplements, or activities I should avoid or focus on to protect my beta cells?
While no food can cure T1D, your care team can give you personalized advice on nutrition and activities that support your overall health and blood sugar stability.
Tip for your appointment
Write your questions down BEFORE you go. It is easy to forget in the moment.
Bring a notebook or use your phone to take notes during the visit.
If you don’t understand something, always say: “Can you explain that in simpler words?” Good clinicians will always be happy to do this.
You can bring a family member or friend for support and to help remember what was said.
SECTION 5: Treatments That May Help Preserve Beta Cells10-12
Science is moving fast! For decades, the only treatment for T1D was insulin—which manages blood sugar but does not stop the immune attack on beta cells. That is changing. Here is a guide to what is available now and what is coming.
How do these treatments work?
Most beta cell-preserving treatments work on the immune system—they try to calm down or “teach” the immune system to stop attacking beta cells. Some treatments still in development work differently: They try to actually replace the lost beta cells using stem cells.
These treatments are different from insulin. Insulin manages blood sugar. These treatments try to change the root cause—the immune attack itself—while preserving remaining beta cell function.

Additional treatments
In addition to teplizumab, several other therapies, with different mechanisms of action, are currently being developed or studied in clinical trials. Information about these treatments is continually evolving as new research becomes available. For the most up-to-date details on their status, please refer to the resources below or speak with your clinician for more information.10

The big picture on new treatments11,12.
For the first time in history, we have a drug approved to CHANGE the course of T1D (teplizumab).
A new class of treatments is coming—pills, infusions, and cell therapies that may someday free people from insulin injections.
The EARLIER these treatments are given, the better they work. This is why early diagnosis and screening matter so much.
None of these treatments replace insulin right now—they work alongside it.
You do not have to wait passively. Ask your clinician, join screening programs, and consider clinical trials.
Researchers are genuinely close to functional cures. Your participation in research helps make it happen faster.
You are not alone.
Living with T1D—or loving someone who does—is hard. But the science has never been more hopeful. Every year researchers learn more about how to protect beta cells, slow T1D, and restore insulin production. By staying informed, asking questions, and connecting with your care team, you are already doing something powerful.
The future is getting brighter. We are in it together.
This guide is for educational purposes only. It does not replace advice from your healthcare team. Always talk to your clinician before starting or stopping any treatment.
References
- Atkinson MA, Raghavendra MG. Cell Metab. 2023;35.9:1500-1518.
- Haller MJ, et al. Horm Res Paediatr. 2025;97:529-545.
- Diabetes Control and Complications Trial (DCCT) Research Group. Ann Intern Med. 1998;128(7):517-523.
- Fuhri Snethlage CM, et al. Diabetes Care. 2024;47:1114-1121.
- Lachin JM, et al. Diabetes. 2014;63:739-748.
- Limbert C, et al. Diabetes Care. 2023;46(10):1747-1749.
- Quick guide to type 1 diabetes (https://breakthrought1d.org.au/what-is-t1d/quick-guide-to-t1d/). Accessed 3/16/2026.
- American Diabetes Association (ADA). Diabetes Care. 2026;49:S27-S49.
- Centers for Disease Control and Prevention (CDC). Type 1 diabetes (https://www.cdc.gov/diabetes/about/about-type-1-diabetes.html). Accessed 3/16/2026.
- Participate in clinical trials (https://www.breakthrought1d.org/clinical-trials/). Accessed 3/16/2026.
- Simmons, et al. Diabetes Technol Ther. 2023;25(11):790-799.
- Ramos EL, et al. N Engl J Med. 2023;389.23:2151-2161.