Clinical Presentation and Natural History of T1D
Type 1 diabetes (T1D) is a slowly progressive disease. It may take months or even years before symptoms severe enough for diagnosis develop, and by then patients are typically in a clinical crisis. However, multiple autoantibodies may be detected from a few weeks up to 20 years before the onset of clinical disease.1 Indeed, 90% of children who develop T1D before puberty have islet autoantibodies (IAbs) by 5 or 6 years of age, and many have IAbs by 2 years of age.2
The most common presentation of T1D in children is absolute insulin deficiency, leading to diabetic ketoacidosis (DKA), which has higher rates in African American and Hispanic children.3
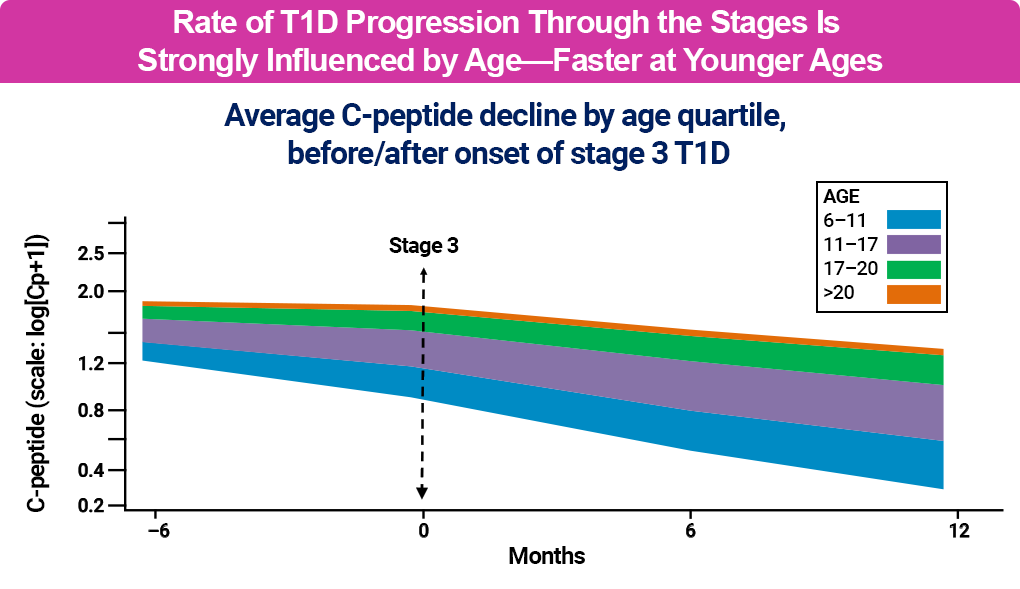
The rate of β-cell destruction can vary significantly on both an individual level and across populations and age groups, with significantly faster progression at younger ages.1,6
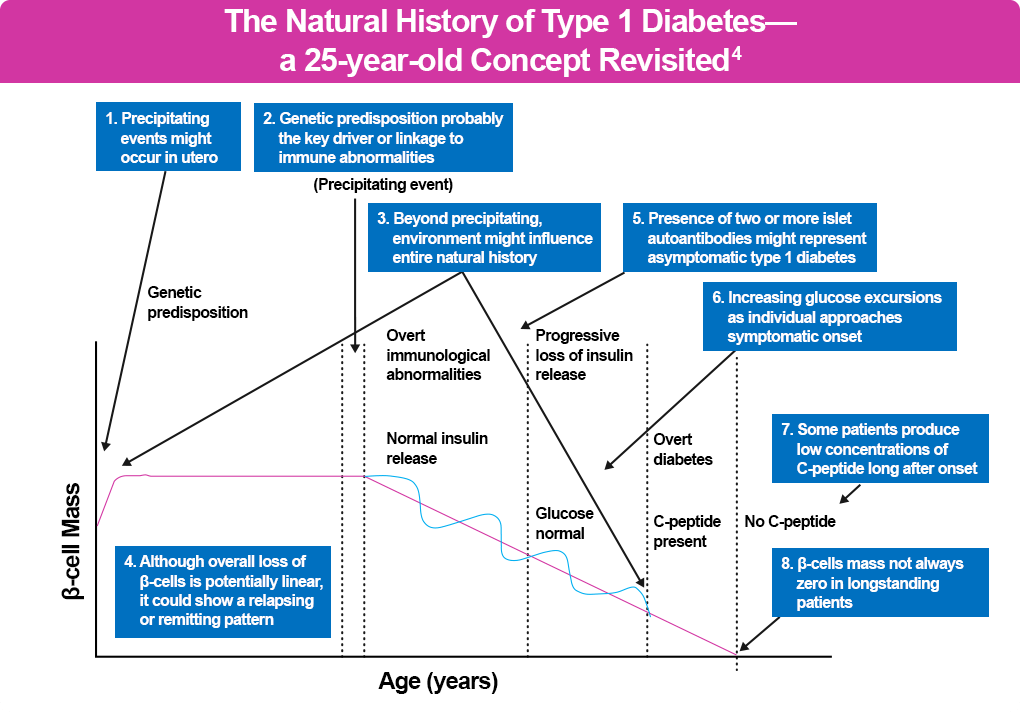
It also differs between individuals, with environmental, physiological, and genetic factors determining functional β-cell mass and C-peptide levels, a marker of endogenous insulin production.1,4 A model about T1D natural history, originally proposed in 1986, describes a somewhat linear concept of progression, from genetic predisposition to a progressive loss of insulin release and development of T1D, and is shown in black in the figure below.4 However, recent research suggests a heterogeneity of the natural history and progression of T1D, which is noted in blue in the figure below, and has improved our understanding of T1D progression and opportunities for asymptomatic screening, early detection, and early treatment.4
References
- Ilonen J, Lempainen J, Veijola R. The heterogeneous pathogenesis of type 1 diabetes mellitus. Nat Rev Endocrinol. 2019;15:635-650.
- Ziegler A-G. The countdown to type 1 diabetes: when, how and why does the clock start? Diabetologia. 2023;66:1169-1178.
- American Diabetes Association. 2. Diagnosis and classification of diabetes: standards of care in diabetes 2025. Diabetes Care. 2025;48(suppl 1):S27-S49.
- Atkinson MA, Eisenbarth GS, Michels AW. Type 1 diabetes. Lancet. 2014;383:69-82.
- Besser REJ, Bell KJ, Couper JJ, et al. ISPAD clinical practice consensus guidelines 2022: stages of type 1 diabetes in children and adolescents. Pediatr Diabetes. 2022;23:1175-1187.
- Greenbaum CJ, Bean CA, Boulware D, et al. Fall in C-peptide during first 2 years from diagnosis: evidence of at least two distinct phases from composite Type 1 Diabetes TrialNet data. Diabetes. 2012;61(8):2066-2073.